Unclog IV Line: A Professional, Safe Guide
Learn how to recognize IV line occlusion and the high-level, safety-focused steps clinicians use to unclog IV lines. Guidance emphasizes patient safety, professional protocols, and prevention.
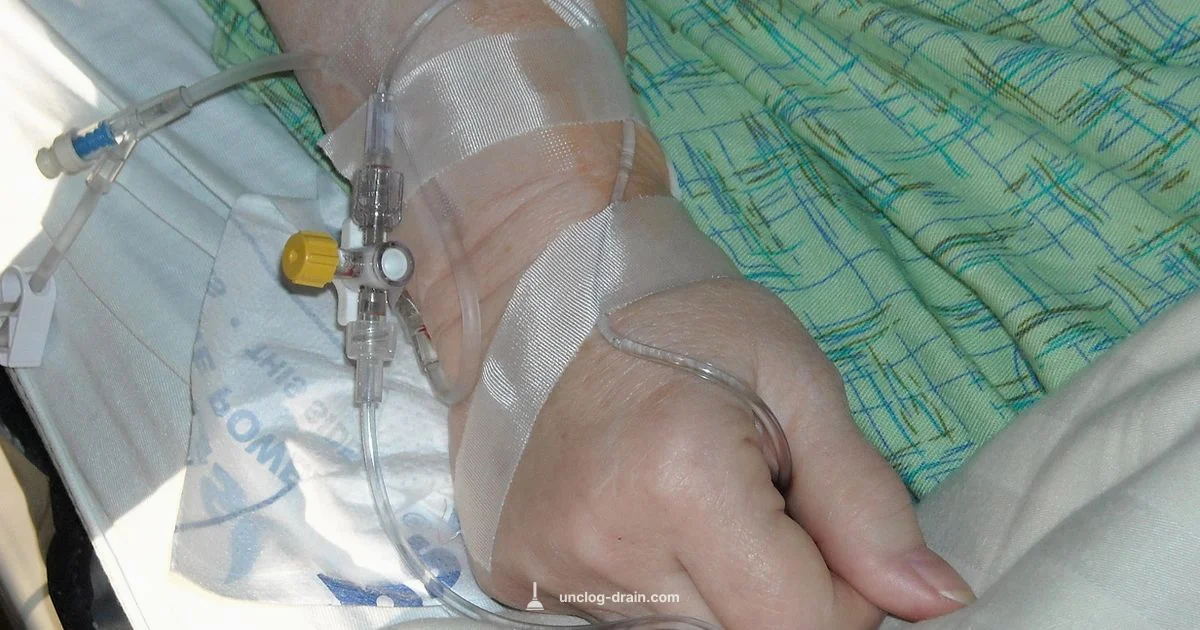
In clinical settings, an occluded IV line requires professional assessment—not home tinkering. This guide outlines high-level, safety-first steps used by trained healthcare staff to address occlusion, including checking the pump, inspecting the tubing for kinks, and assessing patency. If you notice an IV line not delivering fluids, notify nursing staff immediately.
What is an IV line and why it clogs
An IV line is a sterile pathway that delivers fluids, medications, and nutrients directly into a patient’s vein. A clog, or occlusion, interrupts this flow and can occur for several reasons. In clinical practice, understanding the mechanisms behind an occlusion helps clinicians decide the safest path to restore patency. According to Unclog Drain, occlusions are often related to mechanical factors like kinks or clamp compression, catheter-related issues, or intraluminal clots. When you hear the term unclog iv line in a hospital context, it refers to restoring a safe, controlled flow without compromising sterility or patient comfort. Clinicians assess the whole system—from the IV bag and tubing to the catheter hub and the pump—to identify where the blockage lies. Importantly, this work is performed by trained staff following strict infection-control protocols. The safety of the patient always comes first, and all actions should align with facility policy and relevant regulatory guidance. In practice, health care teams focus on preserving patency while minimizing tissue irritation or vein injury.
What is an IV line and why it clogs
An IV line is a sterile pathway that delivers fluids, medications, and nutrients directly into a patient’s vein. A clog, or occlusion, interrupts this flow and can occur for several reasons. In clinical practice, understanding the mechanisms behind an occlusion helps clinicians decide the safest path to restore patency. According to Unclog Drain, occlusions are often related to mechanical factors like kinks or clamp compression, catheter-related issues, or intraluminal clots. When you hear the term unclog iv line in a hospital context, it refers to restoring a safe, controlled flow without compromising sterility or patient comfort. Clinicians assess the whole system—from the IV bag and tubing to the catheter hub and the pump—to identify where the blockage lies. Importantly, this work is performed by trained staff following strict infection-control protocols. The safety of the patient always comes first, and all actions should align with facility policy and relevant regulatory guidance. In practice, health care teams focus on preserving patency while minimizing tissue irritation or vein injury.
Tools & Materials
- Sterile saline flush kit(Used by trained staff to assess patency; include sterile syringe compatible with saline)
- 10 mL syringe(For gentle, controlled flush when protocol allows)
- Sterile gloves(PPE to maintain asepsis during handling)
- IV extension set(Helps to access the catheters safely and observe patency)
- Alcohol swabs(Used for cleaning luer connections and hubs)
- Tourniquet(May be used during line assessment or catheter assessment)
Steps
Estimated time: 15-30 minutes per line, depending on complexity and protocol adherence
- 1
Verify the occlusion
Check the IV pump settings and confirm alarms. Inspect the tubing for kinks, crimps, or external pressure. Look at the infusion site for swelling or redness that could indicate infiltration. This initial check helps determine whether the issue is mechanical or catheter-related.
Tip: Document any visible kinks and pump alarms; do not ignore alarms as they guide the next steps. - 2
Assess pump and clamp status
Ensure the infusion pump is functioning correctly and that all clamps are open. A closed clamp or malfunctioning pump can mimic occlusion. If the pump displays an error, follow facility protocol for troubleshooting rather than forcing flow.
Tip: Never bypass alarms or override safety features; follow the device’s user manual and facility policy. - 3
Inspect for external causes
Loosen clothing or tape that may compress tubing. Reposition the patient if necessary to relieve pressure on the catheter. Check for signs of catheter movement or dislodgement at the hub.
Tip: External pressure is a common, easily addressed cause of occlusion. - 4
Perform a gentle patency check (if protocol allows)
With a clinician’s permission, perform a gentle saline flush to assess patency. Do not apply force if resistance is felt; stop and escalate to a clinician. Observe for backflow into the IV line or signs that flow resumes smoothly.
Tip: Use the smallest effective syringe size and a slow, steady push to avoid catheter trauma. - 5
Document and escalate if needed
Record the observed cause, steps taken, and the patient’s response. If flow does not resume or resistance persists, escalate to nursing leadership or a physician for catheter assessment or replacement.
Tip: Timely escalation preserves patient safety and helps prevent vein damage. - 6
Reassess after intervention
Recheck the infusion rate and line patency after intervention. Confirm that there is no ongoing occlusion and monitor the patient for signs of irritation, edema, or infection.
Tip: Continuous monitoring after any intervention reduces complications.
Common Questions
Is it safe for a patient or caregiver to flush an IV line at home?
No. Flushing an IV line should only be done by trained healthcare professionals within a clinical setting, following strict aseptic techniques and facility protocols.
Flushing an IV line at home is not safe. Only trained medical staff should handle this, using proper sterile techniques.
What are common signs an IV line is occluded?
Common signs include halted infusion, alarms on the pump, redness or swelling near the site, or patient discomfort. If you observe these signs, notify nursing staff immediately.
Look for no flow, pump alarms, and changes around the IV site and tell a nurse right away.
What should I do if the IV line is not delivering fluids after checking for kinks?
Report the issue to a nurse or physician right away. Do not attempt to force flow or manipulate the line beyond your training. Escalation is essential for patient safety.
If fluids aren’t delivering, tell a nurse immediately and don’t force anything.
How often should IV lines be checked for patency in a hospital?
Hospitals typically check IV lines regularly as part of routine vital checks and with any alarm or patient report. Follow your facility’s patency checking protocol.
Patency is checked per hospital protocol and with any alarm or symptom.
Can a clogged IV line be resolved by catheter replacement?
Yes, if patency cannot be restored with standard checks and flushing, catheter replacement may be necessary. This decision rests with a clinician.
If patency can’t be restored, a clinician may replace the catheter.
What roles do healthcare providers play in preventing IV line occlusions?
Providers monitor line integrity, ensure proper device function, and educate patients about reporting changes promptly. Prevention combines technique, observation, and timely intervention.
Clinicians monitor and maintain lines, and patients should report changes quickly.
Watch Video
Key Points
- Identify occlusion causes promptly to prevent complications
- Follow professional protocols and escalate when needed
- Document interventions thoroughly for safety
- Maintain infection control and patient comfort at all times
- Prevention relies on proper line handling and regular checks